Introduction
Chronic hepatitis B virus (HBV) infection is a serious public health problem affecting 257 million people worldwide (3.5% of the world population), according to World Health Statistics 2015 by the World Health Organization (WHO) (1). In Turkey, approximately 3.3 million people (4.57% of the population) are considered HBsAg (hepatitis B surface antigen) positive (2). A study published by Tosun et al. has recently reported HBsAg positivity of 1.1% from 22 provinces and seven regions of Turkey (3).
More than one-third of chronic hepatitis B infections occur due to transmission from mother to infant (4). The infection usually occurs in early childhood, especially in high endemic regions with HBsAg prevalence of more than 8% (5, 6). A routine infant and childhood immunization program for HBV is essential for controlling the prevalence of hepatitis B and its associated complications (7). Therefore, the WHO developed a hepatitis B immunization strategy to prevent chronic hepatitis B infections in 2001. This strategy includes childhood immunization, prevention of transmission from mother to her infant, and immunization of older age groups (8).
In 1995, the hepatitis B vaccine was recommended to be included in the national vaccination program in countries where the HBsAg prevalence was 8% or higher by the Global Advisory Group of the Expanded Program on Immunization, and in 1997 all countries were included in this recommendation. The Ministry of Health in Turkey introduced the hepatitis B vaccine into the national immunization program in 1998 (9, 10). In 2008, the Extended Vaccine Program Memorandum was released to reduce the prevalence of hepatitis B to less than 0.001% in children under five years by 2010 (11).
Three studies published between 2013-2022 have shown HBsAg positivity rates of 3.5%, 1.1%, and 0.3% among people born in 1998 and after in Turkey, respectively (3, 12, 13). Although it has been nearly three decades since the HBV vaccine was included in the national vaccine program, the number of comprehensive studies related to seroprevalence in the population, including adults and the pediatric population, is low in our country. Therefore, the present study aimed to evaluate the rate of HBsAg and anti-HBs (antibodies to hepatitis B surface antigen) in people born in 1998 and after in Şırnak, a province in south-eastern Turkey. We evaluated the changes in the hepatitis B infection rates in the region over twenty years and determine the hepatitis B immunity rates after the national immunization program covered hepatitis B.
Materials And Methods
Patients who applied to different outpatient clinics in the province between April 2017 and June 2018 and who were born in 1998 or after were evaluated retrospectively. Patients who were screened for HBsAg and anti-HBs for various reasons, such as pre-operative or school enrolment tests, were included in this study. The data regarding HBsAg and anti-HBs was obtained from the hospital information management system.
The Elecsys HBsAg II assay (Roche, Mannheim, Germany) and the Elecsys anti-HBs II assay (Roche, Mannheim, Germany) were evaluated by patients’ tests and using the ELISA technique. Patients with anti-HBs levels higher than 10 IU/mL were considered positive.
They were divided into four groups according to their ages, 0-5, 6-10, 11-15 and 16-20. HBsAg and anti-HBs positivity rates, HBsAg positive patients’ genders and ages, and positivity rate by age groups of anti-HBs patients were investigated; groups were compared with each other.
The Ethics Committee of İstanbul Medipol University approved the study on November 11, 2022, with the decision number E-10840098-772.02-6792.
Statistical Analysis
The statistical analyses were performed using the Statistical Package for Social Sciences (SPSS) 22.0 (IBM Corp., Armonk, NY, USA). Pearson’s chi-square test was used to compare the differences in the categorical variables among the groups.
Results
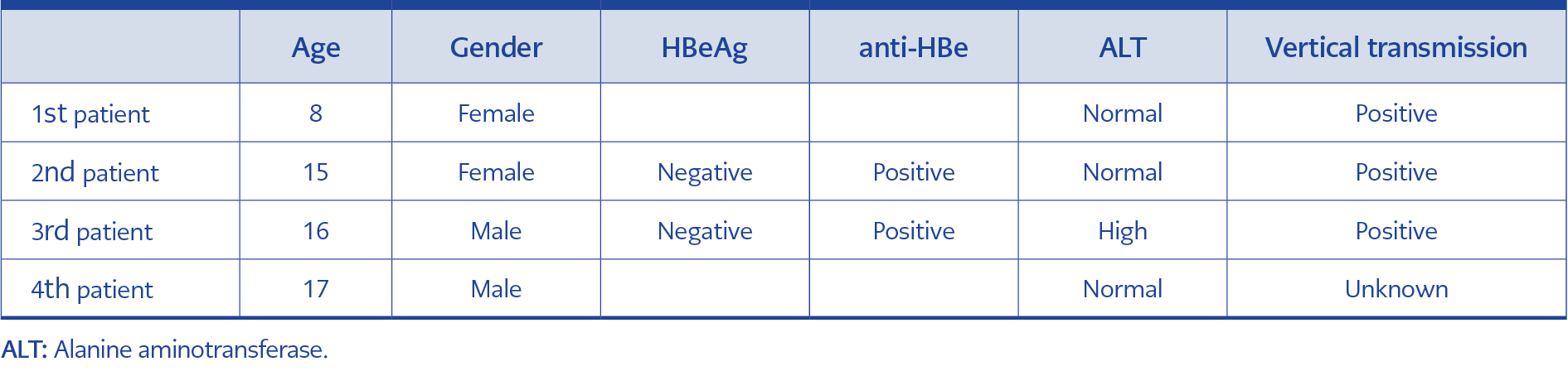
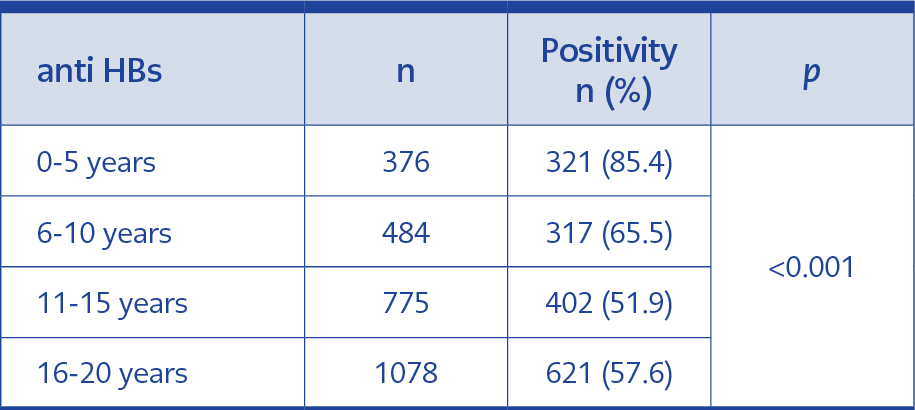
Of 2713 patients, 1530 (56.4%) were male, and the mean age was 12.77 (0-20). Four patients (0.14%) were positive for HBsAg (Table 1). HBsAg was detected in the mothers of three patients (75%). The anti-HBs positivity rate was 61.22%. There was a statistically significant difference regarding the anti-HBs positivity rate between the groups (p<0.001). The anti-HBs positivity rate was higher in the 0-5 and 6-10 age groups. In addition, the difference was statistically significant (p<0.001) when patients were divided into two age groups, 0-10 and 11-20 years old. The anti-HBs positivity rate of patients in the 0-10 age group (74.2%) was significantly higher than in the 11-20 age group (55.2%) (Table 2).
Discussion
In our study, the HBsAg positivity rate was detected as 0.14%, and it was observed that the rate of hepatitis B has significantly reduced in the individuals born in 1998 and after (2). The rate of anti-HBs in this study (61.22%) was approximately double the anti-HBs positivity rate (31%) found in previous studies conducted on the population of Turkey (14).
In a study conducted to evaluate HBsAg and anti-HBs positivity between individuals born between 1976 and 1997, the HBsAg positivity rate was measured as 6.1% in the general population of Turkey. Other studies conducted on children born in 1997 or after in different regions of Turkey measured the positivity rate between 0.16% and 1.25% (15-18). Two studies on adults living in southeast Turkey between 2000 and 2018 found the HBsAg positivity rate as 8% and 1%, respectively (19, 20). Our study showed that the HBsAg positivity rate was 0.14% in individuals born in 1998 and after, pointing out a significant reduction in HBsAg rates after 1998. This result was attributed to the strategies, including the introduction of the hepatitis B vaccine to the national immunization program in 1998, the application of the hepatitis B vaccine and immunoglobulin to the babies born from hepatitis B-infected mothers, and the vaccination of seronegative individuals in older ages.
Studies on the positivity rate of anti-HBs conducted between 1976 and 1997 on the general population of Turkey show the result was 34.6% (15). A recent study in this region showed 27.8% of anti-HBs positivity in adults (20). The studies conducted on children born in 1997 and after in different regions of Turkey indicate an anti-HBs positivity rate between 61.1% and 83.3% (16, 17). The studies on anti-HBs positivity in our country show that the rate has increased in children compared to adult groups. However, when various studies conducted in different regions of Turkey were evaluated, it was observed that the rate of anti-HBs positivity in individuals under the age of 20 in our region is at the lower limit (61.22%). We associated this situation with the fact that studies on children conducted in Turkey have usually targeted younger population than our patients, that there is a low sociocultural level in the southeast region, that migration has increased, and that people living in these regions not having easy access to medical services and that keeping records and the follow-up is difficult.
The hepatitis B vaccine in the universal immunization program provides 90-95% protection and prevents HBV infection for at least 13 years in immunocompetent individuals. However, studies conducted in recent years show a decrease in anti-HBs titer over the years (21-23). In Taiwan, the hepatitis B vaccine was introduced into the national immunization program in 1984, and a study conducted in 1989 showed that the rate of anti-HBs positivity in children at the ages of 1-2, 3-4, and 5-6 was 84%, 23%, and 20%, respectively (24). Another study conducted in Yemen compared the average anti-HBs levels of children between the age of 1-5 and found the highest level in children under the age of 1 (189.3 IU/mL) and the lowest level (21.2 IU/mL) in 4-5 (25). In our patients, the anti-HBs positivity rates in the age groups of 0-5, 6-10, 11-15, and 16-20 were determined as 85.4%, 65.5%, 51.9%, and 57.6%, respectively. Literature suggests a negative correlation between age and anti-HBs positivity, and similarly, our study showed that as age decreases, the positivity rate increases.
Our study has a limitation. Because this was a retrospective study, we could not perform an anti-HBc IgG test in pediatric patients. Thus, we could not determine whether immunization for HBV was achieved by vaccination or by acquiring the disease. However, we observed a significant increase in anti-HBs levels after implementing a routine immunization program.
In conclusion, a significant reduction was noted in the rates of HBsAg in southeast Turkey after the hepatitis B vaccine was introduced into the routine immunization program. The hepatitis B vaccine in childhood is the safest method for prevention against HBV-related cirrhosis and hepatocellular cancer. The widespread introduction of hepatitis B vaccination is recommended in Turkey, considering geographical and sociocultural diversity.