The COVID-19 pandemic has been associated with a higher incidence of skin damage of the hands because of the enhanced infection prevention practices among health care workers. This article aims to share our experience and suggestions with health care workers concerning simple and effective practices to prevent and deal with the deterioration of the skin of the hands that is associated with repeated hand washing and sanitation.
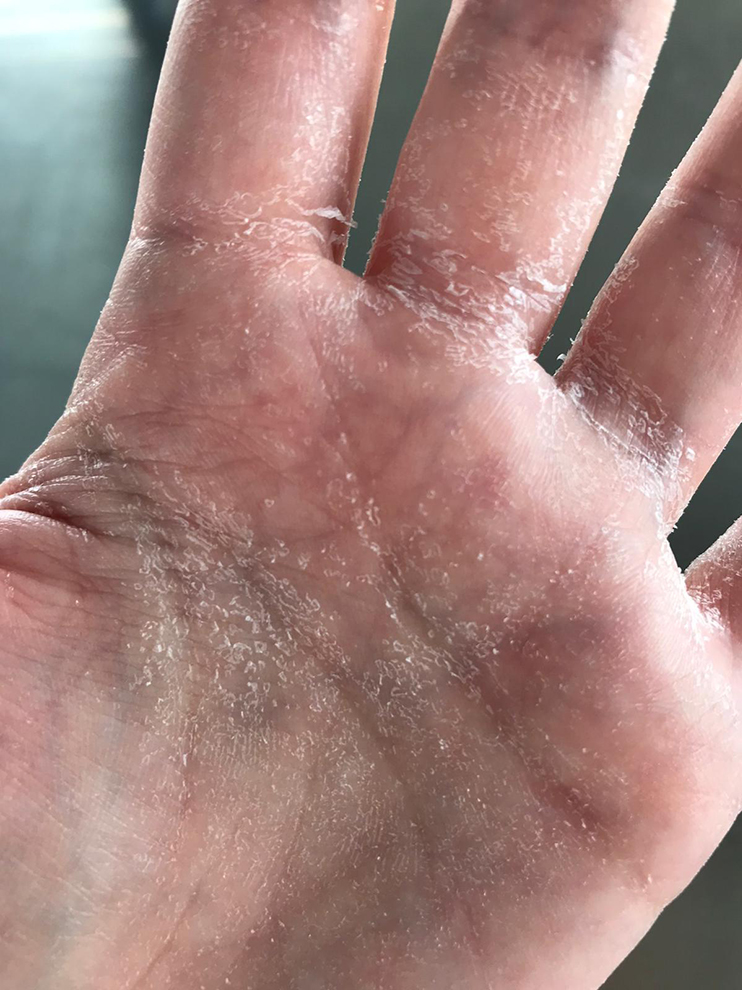
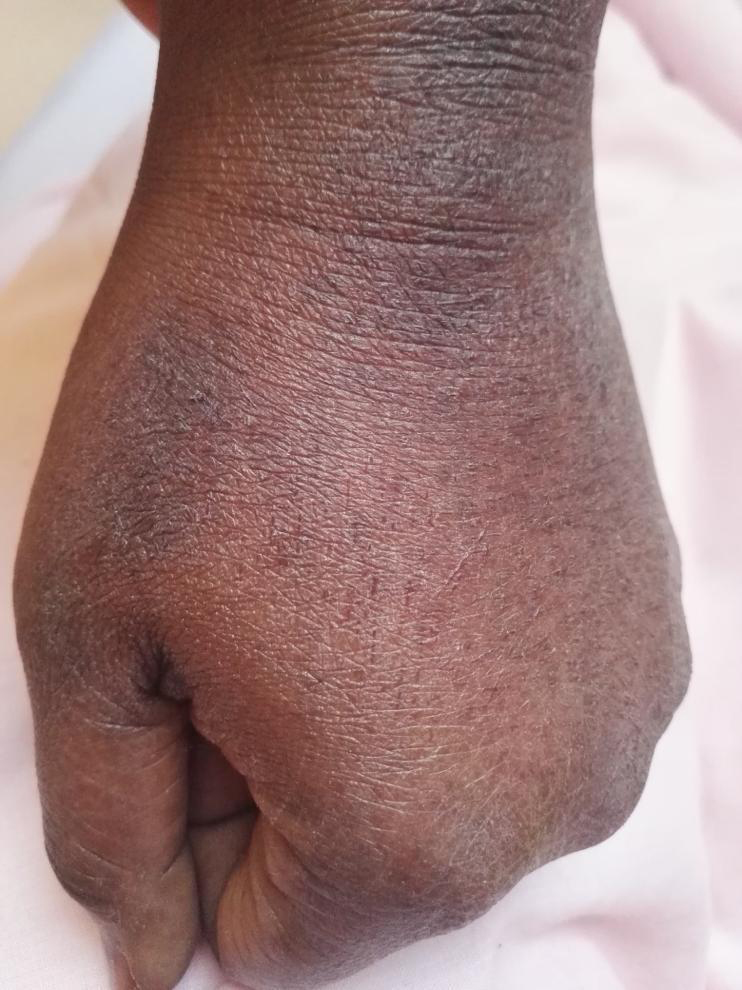
The COVID-19 pandemic puts infection prevention practices on sharp, and appropriate hand hygiene is a cornerstone in controlling further spread of the disease (1). Skin damage associated with the enhanced infection prevention measures related to the COVID-19 pandemic is reported in the literature (2, 3, 4, 5) and our clinical experience, and its incidence is increasing. The prolonged use of aggressive detergents and antimicrobial agents can lead to severe xerosis cutis and fissure-like lesions on the hands and forearms (Figure 1, Figure 2). Such lesions may be painful and can be associated with the leakage of exudative inflammatory secretions. Moreover, the altered state of the skin barrier makes it more vulnerable for irritants and allergens, as well as for infections, which, on its turn, enhances the risk of transmission (6).
Our practice-based suggestion is to use two gloves technique: the healthcare provider should wash their hands and put two pairs of gloves on, one over the other. After that, they should change the pair of gloves on top after having touched a surface and before touching a patient, and vice versa, to minimize the spread of the virus and optimize hand washing. This technique would ensure that the hands of the healthcare provider are always protected by one pair of gloves in direct contact with the skin and that surfaces are minimally contaminated (7). The healthcare provider would then have to wash their hands only at the end of the shift after having removed both pair of gloves.
Moreover, we recommend the regular use of creams with a barrier and moisturizing effect to protect and nourish the hands and forearms’ skin before and after the shift. For many hours, carrying gloves affects the acidity of the skin, making it more prone to external abrasive aggressors such as detergents and microorganisms. (8). Detergents that are not too aggressive towards the skin and free from known allergens should be sought.
Hence, we propose that health care workers who are on the front line should be provided with extraordinary skin protection practices of the hands for prevention and treatment because of the extraordinary challenges posed by this pandemic. We strongly believe that the benefits of our suggestions outweigh the drawbacks of the possible skin maceration that may result from glove-induced chronic occlusion because of the burden related to the etiologic agent of COVID-19.